An advanced drug trial in rats reverses obesity without affecting appetite: ScienceAlert
Phase I clinical trials show promising signs of a new drug that successfully reduced weight and fat mass in obese mice fed a high-fat diet without disrupting their appetite.
If human trials are successful, the drug could revolutionize the treatment of obese people, allowing them to lose weight without losing appetite or avoiding fat.
The drug targets an enzyme found in brain cells called astrocyteswhich can regulate body weight by acting on a distinct group of neurons, according to new research from the Institute of Basic Sciences (IBS) in Korea.
“Previous obesity therapies targeting the hypothalamus have mainly focused on neural mechanisms involved in appetite regulation.” He says IBS neuroscientist Monson SA, first author of the study.
“To overcome this, we focused on non-neuronal astrocytes and determined that reactive astrocytes are the cause of obesity.”
our minds hypothalamus It controls the delicate balance between food intake and calorie burning, and we know that nerve cells in the area connect to adipose tissue and regulate fat metabolism, but exactly how has been a mystery.
In a mouse model of obesity caused by a high-fat diet, the researchers found that activity was significantly reduced in a group called GABRA5 neurons.
So they experimented with reducing the activity of GABRA5 neurons in control mice using chemicals. This resulted in weight gain via decreased heat production (thermogenesis). brown fat and greater white fat storage.
On the other hand, stimulation of GABRA5 neurons in the hypothalamus resulted in significant weight loss in obese mice, suggesting that GABRA5 neurons can function like a reverse switch to control weight.
“We discovered a unique group of fat-burning neurons,” the authors say He writes in their published paper.

Sa and his colleagues were surprised to find that astrocytes were controlling the activity of this group of GABRA5 neurons, switching weight loss on and off. Astrocytes react to disease and injury by releasing chemicals to help protect nerve cells from damage.
They discovered that reactive astrocytes were more common in the brains of obese mice than in mice of healthy weights.
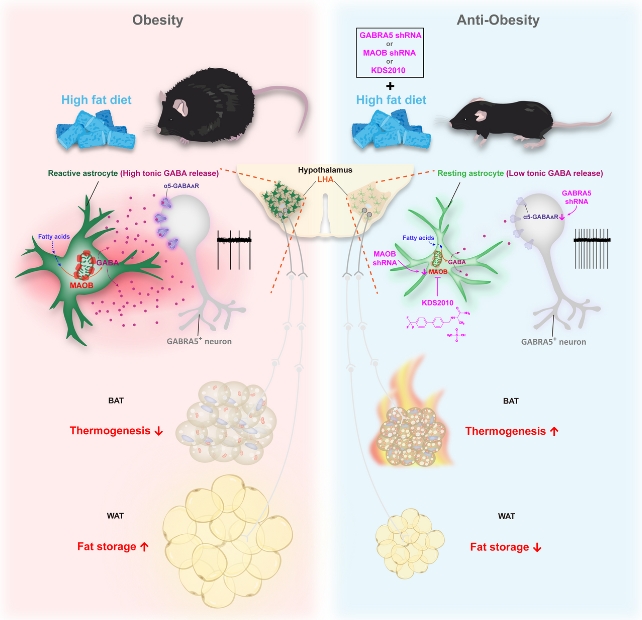
These reactive astrocytes express more of an enzyme called maobwhich produces an inhibitory neurotransmitter called GABA. The increase in GABA is what causes GABRA5 neurons to slow down and stop working properly, which leads to weight gain.
So the team thought that if increasing the activity of GABRA5 neurons reduces fat storage, then preventing astrocytes from producing GABA is a potential molecular target for treating obesity.
This is where the promising new drug comes in. Named KDS2010, it inhibits the enzyme MAOB in reactive astrocytes, thus blocking GABA production and allowing GABRA5 neurons to function normally and promoting weight loss.
KDS2010 treatment achieved remarkable results in obese mice. Their adipose tissue metabolism increased, fat storage decreased, and they lost weight despite being fed a high-fat diet, without affecting their food intake.
This study only tested male mice, so there may be more to learn in further research. We may know more soon, as a biotechnology company called Neurobiogen, affiliated with the research team, is currently conducting phase 1 clinical trials with KDS2010.
“Obesity has been designated by the World Health Organization as an emerging infectious disease of the 21st century,” IBS neuroscientist C. Justin Lee He says.
“We look to KDS2010 as a potential next-generation obesity treatment that can effectively combat obesity without suppressing appetite.”
The study was published in normal metabolism.
Source link





